|
| Jacqueline Abernathy |
Executive Director - Euthanasia Prevention Coalition
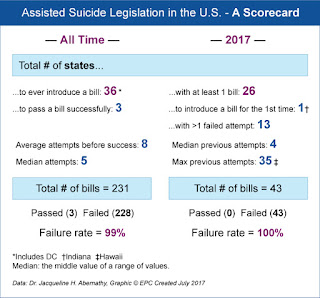
The analysis, to be presented at the 2017 National Euthanasia Symposium in Toronto on October 28, included all bills introduced in 36 states and the District of Columbia since 1994. Of the 231 total bills, nearly one-fifth (43 bills) were introduced just this year in 26 states and all attempts failed. This increase in the number of attempts to legalize assisted suicide is notable due to the fact that such bills have greater than a 99 percent failure rate. Only three have been signed into law in the last 23 years. In spite of the volume of bills introduced this past year, 100 percent of these attempts failed while Alabama tightened their assisted suicide statute.
Only in the last 4 years have any bills passed the legislative process and of the three, only one, Vermont in 2013, was signed into law following standard legislative procedure. California followed in 2015 by resurrecting a defeated bill in an unrelated special session, where processes are abbreviated and legislation is rushed. Similar can be said of Washington DC that recently passed their ordinance through only a city council vote rather than a bicameral legislature. These victories may explain, in part, the staggering increase in the number of bills introduced in other states.
Dr. Abernathy's analysis indicates that while the number of attempts in 2017 alone make up 18 percent of the total number of attempts since 1994, only one state, Indiana, made its first attempt this past year. In 2017, Indiana introduced two bills to legalize assisted suicide alongside the 43 bills in a total 26 states. The other 25 states (or 96 percent) had introduced previous failed assisted suicide legislation. Therefore the analysis shows a potential uptick in the number of bills proposed within each state, there was not a significant increase in the number of new states considering assisted suicide legislation.
Dr. Abernathy also notes that there appears to be no correlation between the number of attempts and an increased likelihood of success. This is in spite of the increase in the number of multiple bills introduced in a single session as well repeat attempts over a number of years. While 12 of the 13 states with previous failed bills introduced more than one bill in 2017, including the one state without previous attempts, historically, the number of bills introduced in one year does not appear to correlate with the likelihood of having a bill pass.
The same can be said of repeat attempts. Vermont introduced a total of 12 bills before the assisted suicide law passed and California proposed 8 but DC had only one proposal. Likewise, Hawaii introduced 5 bills in 2017 alone, adding to a total of 35 failed attempts since proposing its first bill nearly 20 years ago in 1998. Of all 36 states, only Louisiana has only one attempt on record. Over half of all state legislatures that have attempted to legalize assisted suicide have five more attempts and seven of these 19 states have attempts numbering in the double digits. Considering the number of states that continue to fail after exceeding both Vermont and California in both the number of repeat attempts and number of bills per session, this political strategy has yet to suggest that perseverance alone can win sufficient legislative support.
Further analysis should offer more insight but these initial reports demonstrate a continuing overall failure rate of assisted suicide legislation in spite of both recent loses and the significant increase in the frequency of attempts. These initial results do indicate the use of persistence as a political strategy for the assisted suicide lobby but do not validate the efficacy of that strategy. As of yet, these numbers do not suggest lawmakers in general are willing to accept assisted suicide after a certain number of bills are introduced. Perhaps a greater number of lawmakers are willing to introduce bills, but the fact that these bills continue to fail and fewer states are rushing to consider such legislation suggests that assisted suicide remains an unlikely cause to advance in U.S. statehouses.
This article is based on the, yet to be published, analysis of assisted suicide legislation in the U.S. by Dr Jacqueline Abernathy at Tarleton State University.
For more information: